Scarring occurs when the body repairs damage to the skin by producing collagen fibers. Depending on how much collagen is made—and how it’s arranged—the result can be flat, raised, or indented scars.
How does the Skin Heal After Injury or Surgery?
“The wound healing process consists of 4 overlapping phases—hemostasis, inflammation, proliferation, and remodeling… The proliferative phase mainly involves keratinocyte migration, cellular proliferation, and the formation of new blood vessels… The maturational or remodeling phase starts around week 3 and can last up to 12 months. The excess collagen degrades… The maximal tensile strength of the incision wound occurs after about 11 to 14 weeks, but the ultimate scar will only have about 80% of the original strength.” – StatPearls, NIH
If collagen production is excessive or unbalanced, scarring becomes more visible.
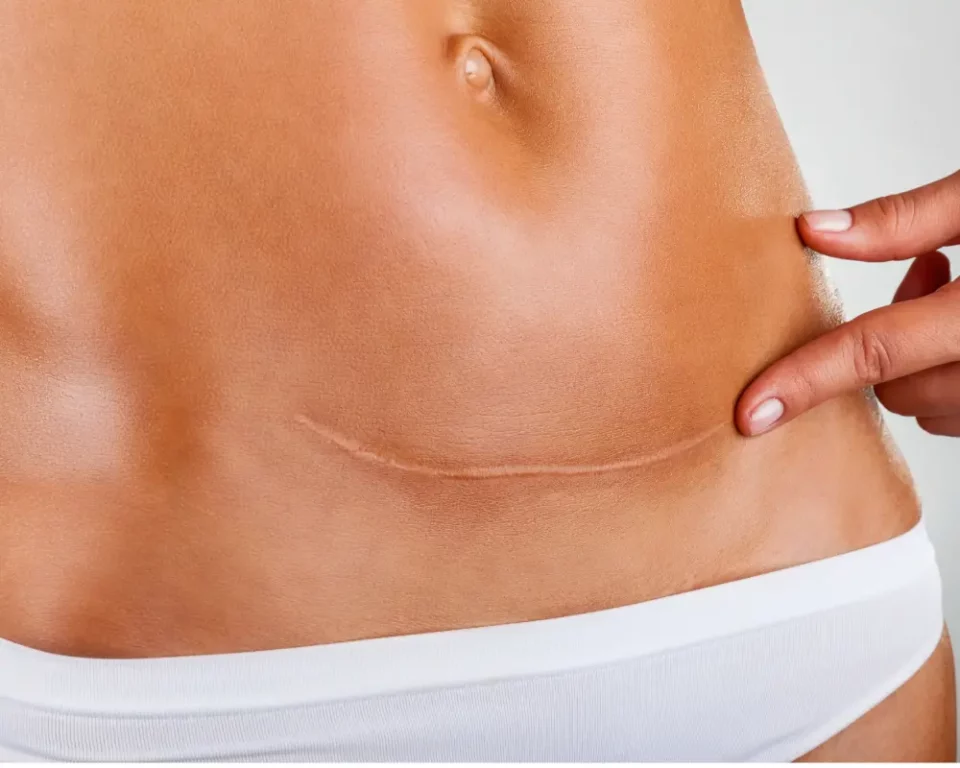
Surgical wounds, including those from procedures like chest or gender-affirming surgery, often heal with prominent lines or raised scar tissue that can evolve differently depending on genetics, location, and aftercare.
Different Types of Scars and Their Patterns
Scars don’t all look the same:
- Atrophic scars – Sunken or pitted scars, often from acne or chickenpox, caused by collagen loss. Also known as acne scars or post-acne scarring.
- Hypertrophic scars – Raised, thickened scars that remain within the wound boundary.
- Keloids – Overgrown scars that spread beyond the original wound site, sometimes seen after surgery or piercings.
- Stretch marks – Linear scars formed when skin stretches too quickly for its elasticity.
- Surgical scars – Linear scars that form after medical or elective procedures. These may flatten and fade, remain raised, or widen depending on how the skin heals.
Common Causes of Scarring
| Cause | How Scars Form | Typical Scar Types |
|---|---|---|
| Acne breakouts | Inflammation damages follicles, leading to collagen breakdown or overproduction. | Atrophic (pitted), hypertrophic |
| Surgical procedures | Incisions trigger collagen repair; scar appearance varies by genetics, care, and tension on the wound. | Linear, hypertrophic, keloid |
| Injuries & cuts | Trauma to skin heals with new collagen fibers that may not align smoothly. | Hypertrophic, keloid, flat |
| Skin picking or scratching | Repeated injury disrupts healing and increases risk of noticeable marks. | Atrophic, hypertrophic |
| Rapid skin stretching | Skin tears at the dermis level as collagen fibers can’t keep up with tension. | Stretch marks (striae) |
| Burns | Heat damages multiple skin layers, producing thick, raised, or irregular scars. | Hypertrophic, keloid |
Why It Matters for Skin Health
Scars are a natural part of healing but can affect self-confidence and comfort. Identifying the type of scar helps guide choices about care and whether treatment is needed for texture, appearance, or sensitivity.
Quick Summary:
- Scars form through collagen response during healing.
- The amount and arrangement of collagen determine scar type.
- Scars can result from acne, injury, surgery, or rapid stretching.
- Understanding your scar type informs long-term skin decisions and care.